
Background
In the United States (U.S.), about 1,278 babies are born with spina bifida (SB) each year, with new care therapies leading to increased life expectancy well into adulthood. However, individuals with SB still face many care challenges affecting their quality and continuity of care. Studies show that the lack of continuity in preparing individuals with SB to transition into adult-focused care may have detrimental health consequences.
A 2017 study by Kelly et al. found that clinics self-rated their ability to provide health care transition services for patients as 5 out of 10. Since this study, both the 2018 Guidelines for the Care of People with Spina Bifida from the Spina Bifida Association (SBA) and the American Academy of Pediatrics (AAP) Clinical Report Supporting the Health Care Transition From Adolescence to Adulthood in the Medical Home have been published.
Following this, in collaboration with the Centers for Disease Control and Prevention (CDC) and the SBA, the AAP designed and implemented a quality improvement learning collaborative on transition in SB care. The project used the Got Transition Six Core Elements of Health Care Transition methodology in conjunction with the clinical guidance available through the SBA and AAP to improve the transition of youth with SB from pediatric to adult-focused care. After two successful cohorts of the learning collaborative, lessons learned were applied to design and implement three cohorts of this ECHO.
Health Care Transition From Pediatric to Adult-focused Care for Youth With Spina Bifida Project ECHO®
This article describes Cohort 3 of a Project ECHO® collaboration between the AAP, the CDC and multidisciplinary SB healthcare clinicians throughout the U.S. to improve structured health care transition for individuals with SB. Project ECHO® (Extension for Community Healthcare Outcomes) is a telementoring program designed to create communities of learners by bringing together healthcare providers (medical officers, general physicians, nurse practitioners, nurses, community health workers, etc.) and experts in topical areas using didactic and case‐based presentations, fostering an “all learn, all teach” approach.
Using widely available videoconferencing technology, clinical management tools and case‐based learning, healthcare providers develop knowledge and self‐efficacy on diseases, conditions and/or processes. It is widely implemented as an evidence-based virtual education model that aims to enhance the capacity of clinicians to manage a range of health concerns.
The AAP developed and implemented an ECHO focused on supporting healthcare providers who care for children with SB to successfully transition youth and young adults from pediatric to adult-focused care systems. The third cohort of the activity occurred between February and May 23, 2024. The objectives of this ECHO were to identify the medical and developmental issues for youth and young adults with SB; increase healthcare clinician competence in the SB health care transition management; and identify strategies to support family engagement and shared decision-making.
Methods
Using an interprofessional approach to healthcare education, the program considered the patient’s needs from multiple socio-medical perspectives. To ensure all aspects of care were considered, the ECHO faculty included a multidisciplinary group of primary care pediatric and internal medicine physicians, subspecialists, a nurse, social workers, a neuropsychologist, an individual with SB and a parent of an individual with SB. Participants from previous cohorts were invited to serve as faculty, thus increasing the circle of experts.
While interprofessional education has become more common, incorporating the patient and caregiver voices into the design and delivery of the initiative is less common. One of the social worker faculty lives with SB and was involved in the design of the program from the start. This faculty member offered the unique lived experience of having transitioned from pediatric to adult care, as well as her professional experience as a care coordinator providing support for individuals with SB in the adult clinic.
Each ECHO session included a brief lecture by a subject matter expert followed by participant presentations of deidentified patient cases to receive guidance and knowledge on their actual cases that they could implement immediately. Participants completed a post-program survey (utilizing a retrospective pre-post design), and, in Cohorts 1 and 2, focus groups at the conclusion of the ECHO. The activity was designed using Malcolm Knowles’ Five Principles of Andragogy, specifically by ensuring the learning was experiential, relevant to the learners’ current roles, and that the instruction was problem centered.
Findings and Takeaway
Multidisciplinary teams at SB clinics and pediatric practices that serve patients with SB were engaged, with a total of 111 unique participants over three cohorts.By expanding continuing education credentials in each cohort, the ECHO successfully engaged more of the multi-disciplinary healthcare clinic team. ECHO participants included physicians, nurse practitioners, psychologists, urologists, nurses, social workers, care coordinators and parents of children living with SB. Cohort 3 included 44 unique participants from 29 institutions across 17 U.S. states and Canada.
The evaluation assessed improvements in healthcare provider education using Moore’s Levels of CME Outcomes as a framework. Moore’s Levels 1–5 were measured, covering participation, satisfaction, knowledge, confidence and practice change outcomes:
- Moore’s Level 1 (Participation): Included demographic and attendance data.
- Moore’s Level 2 (Satisfaction): Assessed the extent to which participants’ expectations regarding the format and content of ECHO sessions were met.
- Moore’s Levels 3 and 4 (Knowledge and Confidence): Evaluated participants’ knowledge gains (the degree to which they could articulate program objectives) and their confidence in applying this knowledge in practice, such as managing health care transitions for youth and young adults with SB.
- Moore’s Level 5 (Performance): Measured the extent to which the ECHO program led to practice-level or performance changes.
All levels were assessed using self-reported survey measures. While patient outcomes (Moore’s Level 6) and population health (Moore’s Level 7) were not directly measured in this evaluation, the emphasis on provider performance and confidence offers an indirect indication of potential improvements in SB patient care and broader population health outcomes over time.
The ECHO program successfully achieved its goals. Attendance (Moore’s Level 1) was strong, as previously reported above, and participant satisfaction (Moore’s Level 2) was rated highly, as indicated by responses to self-reported survey questions (Figure 1). The retrospective pre-post survey demonstrated statistically significant improvements in participants' knowledge and confidence (Moore’s Levels 3 and 4) in managing health care transitions for youth with SB (Figure 2). Participants reported that their knowledge and confidence in key areas, such as transition planning and implementing best practices, had markedly increased after completing the program.
Furthermore, the program achieved its desired outcomes in performance improvements (Moore’s Level 5). All respondents to the post-program survey indicated plans to implement changes in their clinical practice based on the knowledge and skills gained from the activity. These planned changes included the adoption of new transition protocols, the creation of resource packets for patients and families, and the integration of evidence-based practices into routine care. The evaluation demonstrated that the AAP SB Cohort 3 ECHO program successfully met its objectives by enhancing healthcare provider competence and fostering intentions to implement meaningful practice changes, thus achieving the desired outcomes at Moore’s Levels 4 and 5.
Figure 1. Participant satisfaction (Moore’s Level 2) was assessed using multiple questions, including those shown below, with ratings captured on a 5-point Likert scale (1 = poor, 5 = excellent). Cohort 3 participants who completed the post-program survey (n=13) rated their experience highly, with all responses categorized as "Good" or higher, demonstrating strong satisfaction across the evaluated domains.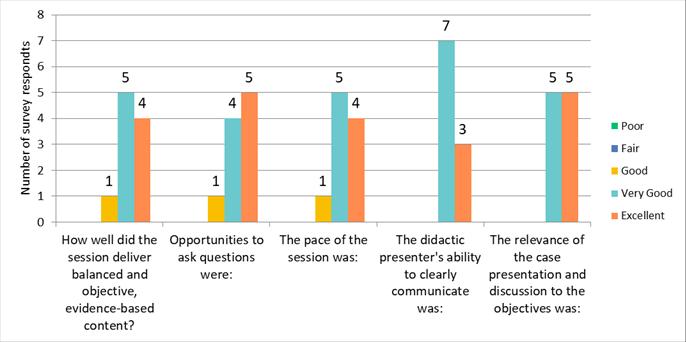
Figure 2. Knowledge and confidence (Moore’s Levels 3 and 4) was assessed through participant ratings of 12 learning objectives on a 5-point Likert scale (1 = no skill, 5 = expert). 11 out of 12 objectives showed significant increases (p<0.05) from pre- to post-ECHO among Cohort 3 participants who completed the post-program survey (n=13).
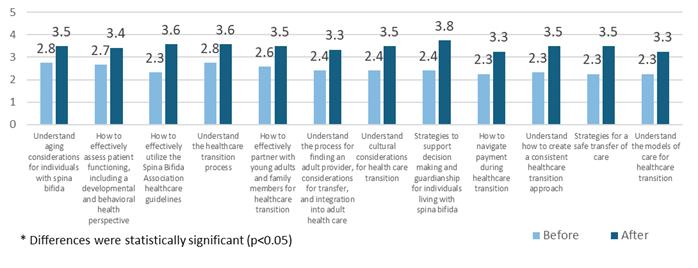
Conclusion
This ECHO program successfully achieved its goals of enhancing knowledge, confidence and practice-level changes among healthcare providers in SB health care transition management. By asking participants to share deidentified cases for discussion, the program therefore harnessed the collective wisdom of the group. This method also ensured the learning was directly applicable to each participant’s role and was problem-based.
The design of this activity specifically addressed a systemic issue of the difficulties experienced by individuals with SB as they age out of pediatric care and are required to navigate the adult healthcare system. These gaps were identified through participant surveys and focus groups. Learners were encouraged to identify their own knowledge and competency gaps and to problem-solve as a healthcare team, rather than in their own individual roles. Additionally, AAP Accreditation Services was involved in the planning and development of the activity to ensure the multidisciplinary audience would be able to receive their respective credits and that the standards of each accrediting body were met. This program was accredited by the Accreditation Council for Continuing Medical Education, the American Nurses Credentialing Center and the National Association of Social Workers.
Funding
This ECHO program was developed through the support of cooperative agreement #5NU38OT000282 between the AAP and the Centers for Disease Control and Prevention’s National Center on Birth Defects and Developmental Disabilities.